Duration
5:00 minutes
Category
Stem cell therapy
Series
Cord blood banking
Objective
Educational
Immunity, infections and vaccines
What you will learn
- What is immunity?
- How vaccines work
- Types of immunity
- Developing the strength of the immune system
This lesson delves into the intricacies of the immune system and how humans naturally acquire immunity through encounters with pathogens or vaccinations.
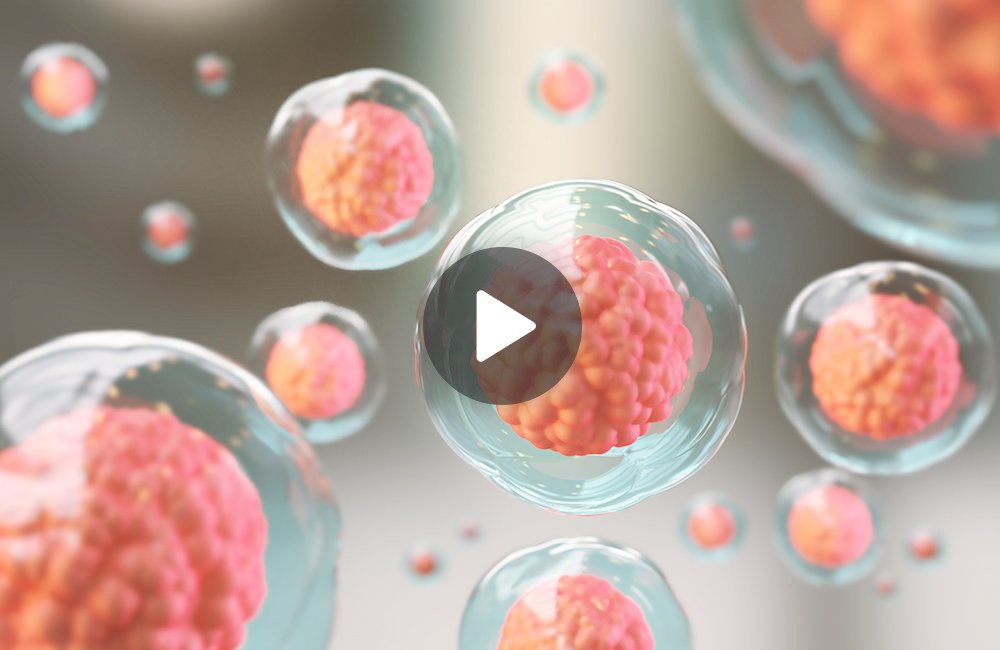
On a daily basis, we come into contact with various pathogens like bacteria and viruses in our surroundings. The ability of our body to identify these invaders and eliminate them is crucial. This concept encapsulates immunity – the immune system’s capacity to identify and neutralize pathogens before they can wreak havoc within our bodies.
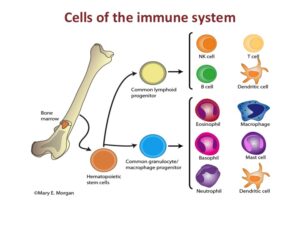
The human immune system is a complex entity involving multiple organs. In this discussion, our focus will center on one integral component of the system: immune cells.
The immune system comprises a multitude of distinct immune cells, each carrying out specific roles in the immune response. All of these cells originate from a single kind of stem cell known as a hematopoietic stem cell.
Within the body, hematopoietic stem cells are situated within the bone marrow. Additionally, cord blood serves as an additional source of these stem cells.
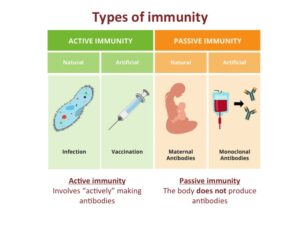
Immunity can be developed through two main mechanisms: active immunity and passive immunity.
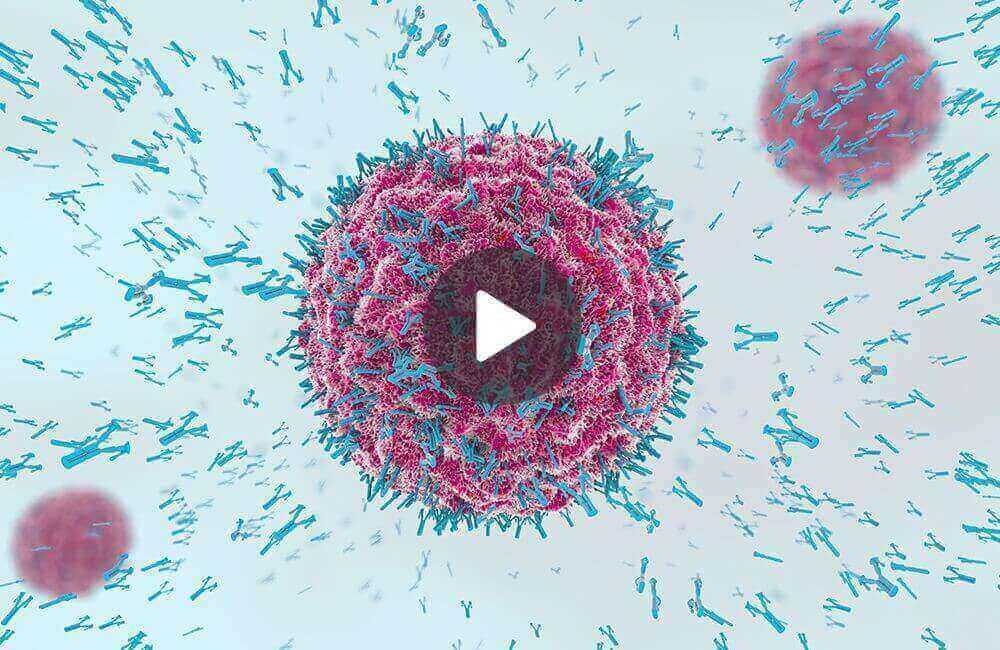
One facet of active immunity involves the production of antibodies – large Y-shaped proteins employed by the immune system to identify invaders. These antibodies can emerge as a response to an infection or after receiving a vaccine.
In passive immunity, the focus is not on creating antibodies but rather on transmitting them. A natural instance of acquired passive immunity is the transfer of antibodies from mother to child through breast milk.
Artificial acquisition of passive immunity involves infusing a blood sample from an individual possessing antibodies for a specific infection into someone who can’t generate their own antibodies.
Vaccines exemplify a method of fostering active immunity. Vaccines can be formulated in various ways, containing either a deceased or weakened form of a pathogen, a pathogen-produced toxin, or a protein from the pathogen’s surface.
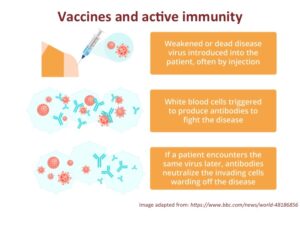
Upon receiving a vaccine (such as one for influenza), the inactivated or weakened pathogen enters the body. This prompts the immune system to identify the foreign invader and signal white blood cells to produce antibodies capable of combating the ailment.
Consequently, the body generates a set of antibodies specific to the encountered pathogen. This equips the body to recognize and neutralize the pathogen in case of future encounters. Essentially, immunity to the particular pathogen from the vaccine is established.
With time, our immune memory accumulates, leading to an increased number of antibodies against diverse diseases or a broader repertoire of antibodies targeting different diseases.
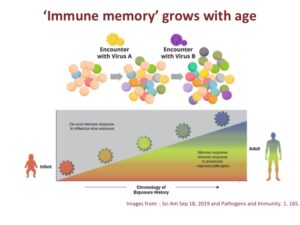
Initially, we possess a limited pool of antibodies. As we experience our first viral infection – let’s say virus A – antibodies against virus A are generated.
Subsequently, virus B comes into the picture. New antibodies are then created to recognize virus B. This progression continues, ultimately furnishing the immune system with antibodies capable of identifying both virus A and virus B.
This cycle recurs with each new pathogen encounter. Consequently, our immune system strengthens over time due to continuous exposure to various microbes. However, aging brings about changes in the immune system, influencing our ability to respond to infections. To learn more about the influence of age on the immune system, refer to our upcoming lesson on the immune system and aging.
More topics you might like
Continue your journey by selecting another topic.
An introduction to stem cells
What are newborn stem cells and why are they important?
3:45 minutes | Stem cell basics
The immune system and aging
Find out more about how our immune systems change with age
4:30 minutes | Stem cell therapy
Can the aging immune system be rejuvenated?
Exploring ways to restore immunity
6:00 minutes | Stem cell therapy